“Why Does Everything Burn?” – A Story That Might Sound Like Yours
You’re in your 20s, 30s, or 40s.
You finally work up the courage to tell your provider:
“It burns when I try to use a tampon.”
“Sex has always hurt.”
“I feel like I’m tearing, even when we use lube.”
Your exam comes back “normal.” You might be told it’s in your head, to relax, or to have a glass of wine first.
But the pain is real. You start to dread intimacy. You avoid tight clothing. You begin to wonder if something is wrong with you.
If this sounds familiar, you’re not alone—and you may be dealing with vulvodynia.
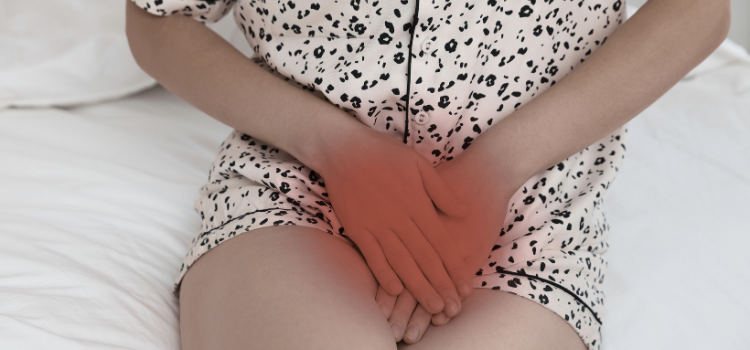
What Is Vulvodynia?
Vulvodynia is chronic vulvar pain (pain of the external genital area) that lasts at least 3 months and doesn’t have a clear cause like an infection, skin condition, or active injury.
People often describe it as:
- Burning
- Rawness
- Stinging
- Sharp, cutting, or tearing pain
- Sandpaper or “knife-like” pain
It may be:
- Localized – often around the vaginal opening (vestibule)
- Generalized – affecting a larger area of the vulva
- Provoked – triggered by touch, sex, tampons, tight pants, sitting
- Spontaneous – present even without touch or pressure
Many patients hear words like vestibulodynia or provoked vestibulodynia—these are specific types of vulvodynia, focused around the entrance of the vagina.
Why Does Vulvar Pain Happen?
There isn’t one single cause. Vulvar pain often shows up as the end result of several factors layering on top of each other over time:
- Pelvic floor muscle overactivity
- The muscles around the vagina can become tight, guarded, or in spasm.
- This creates a cycle of pain → tightening → more pain → more tightening.
- Nervous system sensitivity
- Nerves in the area (including the pudendal nerve) can become irritated or hypersensitive.
- Even light touch (a Q-tip, clothing, finger, or tampon) can feel painful.
- Hormonal or tissue changes
- Birth control, postpartum changes, perimenopause/menopause, or medical treatments can impact tissue thickness, moisture, and sensitivity.
- Past infections, medical procedures, or trauma
- Repeated yeast infections, UTIs, biopsies, surgeries, or a painful first sexual experience can all leave a “memory” in the tissues and nervous system.
- Emotional load of pain
- Anxiety, fear, and shame do not cause vulvodynia—but living with chronic pain absolutely affects your brain’s alarm system and muscle tension. This can intensify symptoms.
You do not need to know exactly which factor “started it all” to get help. What matters is a thoughtful, whole-person approach to calming the pain and restoring comfortable function.
How Pelvic Floor Physical Therapy Helps Vulvodynia
Vulvar pain lives in a complex neighborhood of muscles, nerves, skin, hormones, and the nervous system. Pelvic floor physical therapists are trained to work with this entire region.
At N2 Physical Therapy, a typical course of care may include:
1. A Thorough, Gentle Evaluation
Your first visit isn’t a quick peek and a prescription. It’s a conversation and a collaboration.
We may look at:
- How you sit, stand, walk, and move
- Breathing patterns and how you use your abdominal/pelvic muscles
- Hip, low back, and pelvic alignment or muscle imbalances
- External pelvic floor muscle tension and tenderness
- With your consent, a gentle internal or vestibular (around the opening) exam to assess:
- Specific areas of pain
- Muscle coordination and ability to relax
- Skin and tissue reactions to light touch
You are in charge of what we do and do not assess. Everything is explained, nothing is rushed.
2. Calming the Nervous System and Muscles
People with vulvodynia are often told to “just relax.” But if your muscles and nervous system are already on high alert, that’s not exactly actionable advice.
We use specific strategies to help your body learn to feel safe again:
- Manual therapy
- Gentle internal and external techniques to release trigger points and soften overactive muscles
- Addressing tightness in the hips, glutes, and low back that may be feeding into the area
- Desensitization work
- Very gradual, structured exposure to comfortable touch
- Sometimes using cotton swabs, fingers, or dilators as appropriate
- This retrains the nervous system so “danger” signals become “normal touch” again
- Relaxation and coordination training
- Learning to fully let go of pelvic floor muscles
- Pairing breath, movement, and awareness to break the pain–tightening cycle
3. Tools You Can Use at Home
The goal is not to keep you in the clinic forever. It’s to help you build skills and confidence at home, including:
- Home exercises to support hip and pelvic mobility
- Strategies for bowel and bladder habits that avoid extra strain
- Step-by-step guides, when appropriate, for using vaginal dilators or self-release techniques
- Education about positions, pacing, and communication for more comfortable intimacy
4. Collaborative Care With Your Medical Team
Pelvic floor PT is one piece of the puzzle. You may also benefit from:
- Evaluation for infections, skin conditions, or hormonal changes
- Vaginal moisturizers or lubricants
- Topical medications prescribed by your medical provider
- Counseling or sex therapy to process the emotional impact of pain
We regularly coordinate with your other providers (with your permission) so you’re not left trying to connect the dots alone.
It’s Not “All In Your Head.” And You Don’t Have to Live With It.
If you’ve been told your pain is normal, or you’ve been dismissed or rushed through appointments, please hear this:
- Vulvodynia is real.
- Pain with sex or tampons is not just something you have to put up with.
- Help is available, and pelvic floor physical therapy can be a powerful, evidence-informed part of your healing.
Ready to Talk About Vulvar Pain?
If you’re experiencing burning, stinging, or tearing pain with intercourse, tampon use, or even clothing:
- You deserve to be heard.
- You deserve a plan, not a shrug.
At N2 Physical Therapy, our pelvic health physical therapists create a safe, private space to talk openly about your symptoms, your goals, and your comfort level.

